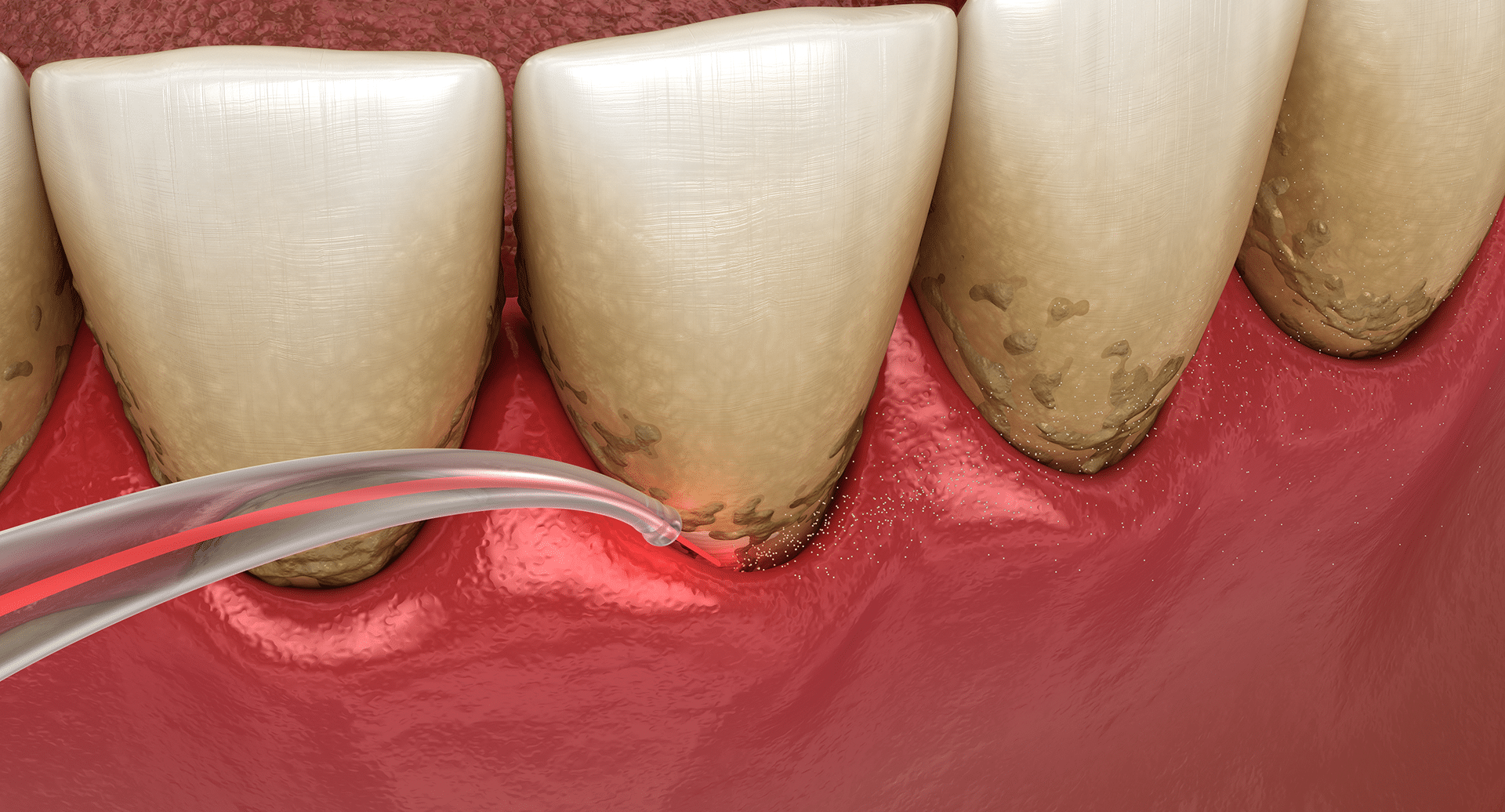
What Is Laser Bacterial Reduction?
KM Admin
Long gone are the days of invasive gum surgery for periodontal disease. With improvements in laser technology, your dentist can effectively combat the bacteria that cause gum disease without incisions or sutures. Learn how laser bacterial reduction works and if it’s an option for you here! How Does Laser Bacterial Reduction Work? Laser Bacterial Reduction...read more

How to Deal With Dental Anxiety
KM Admin
Going to the dentist is crucial for maintaining good oral health. However, for many adults, the thought of a dental visit can be overwhelming due to dental anxiety. Our experienced Alexandria dentist, Dr. Mullaney, explains what causes dental anxiety and provides tips and strategies to overcome your fear. Here’s what you need to know. What...read more
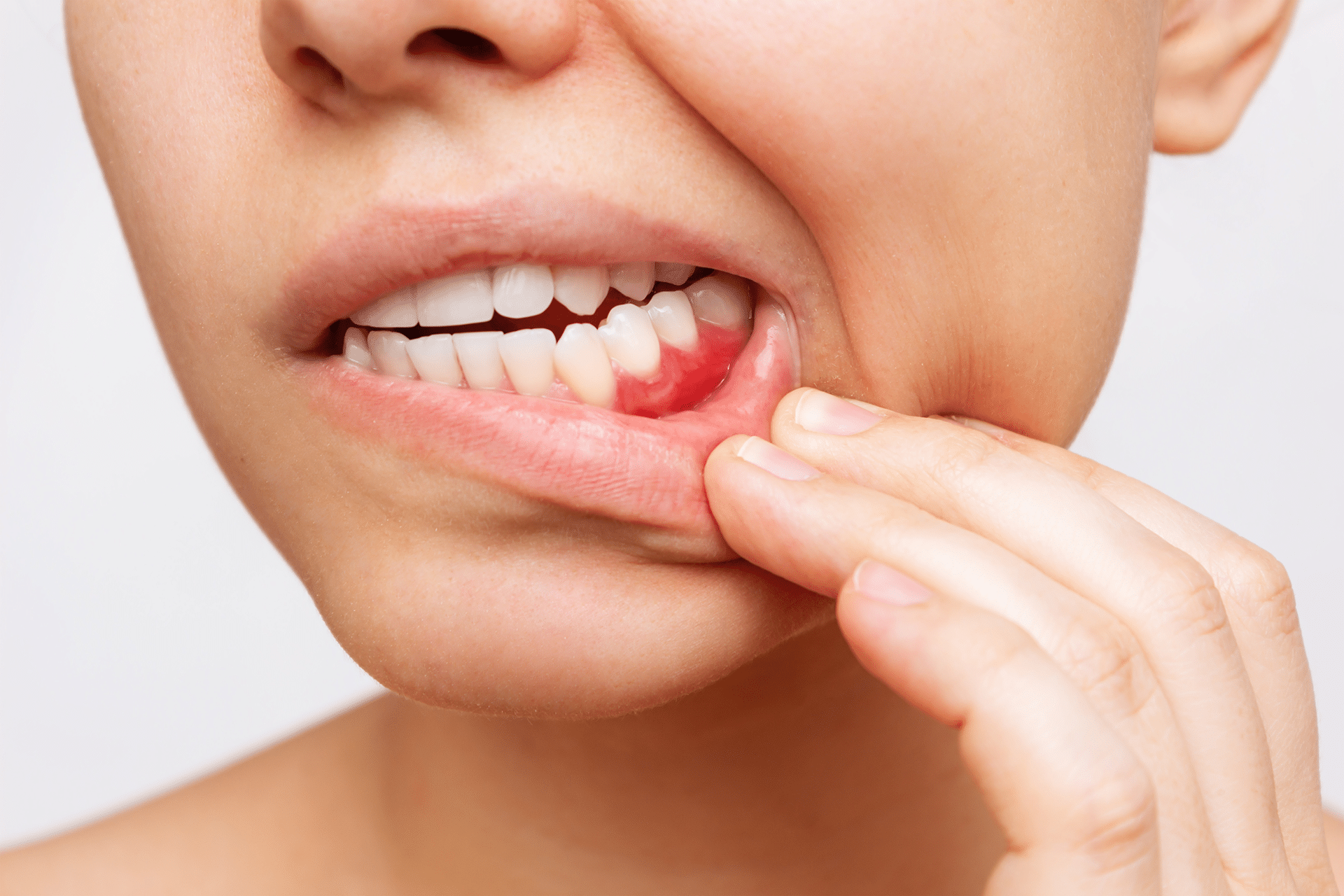
What Is Gum Disease?
KM Admin
Gum disease, also known as periodontal disease, is a common oral health problem that affects people of all ages. It’s estimated that nearly half of adults in the United States have some form of gum disease. Despite its prevalence, many people don’t know what gum disease is, how it can damage their teeth and gums,...read more

Why Do I Need Scaling and Root Planing?
KM Admin
Brushing and flossing are essential for good oral health, but sometimes they’re not enough. If you have an active gum infection, scaling and root planing is a deep cleaning procedure that can help remove harmful bacteria and plaque. Find out what scaling and root planing is, why it’s important, and what to expect during the...read more

7 Signs You Need a Root Canal
KM Admin
Facing a toothache can be distressing, especially when it persists despite over-the-counter remedies and patience. Sometimes, a toothache is more than just a passing discomfort; it may be a sign of infected dental pulp that requires immediate attention. If you’re unsure whether your toothache warrants a root canal, it’s essential to understand the symptoms that...read more

How to Get a Smile Like Meghan Markle
KM Admin
Meghan Markle’s radiant smile has captivated the world, and it’s no wonder why so many people aspire to have a smile like hers. With its perfect alignment and dazzling white color, Meghan’s smile exudes confidence and beauty. If you’ve been dreaming of having a smile like Meghan Markle’s, you’re in luck. Find out the steps...read more
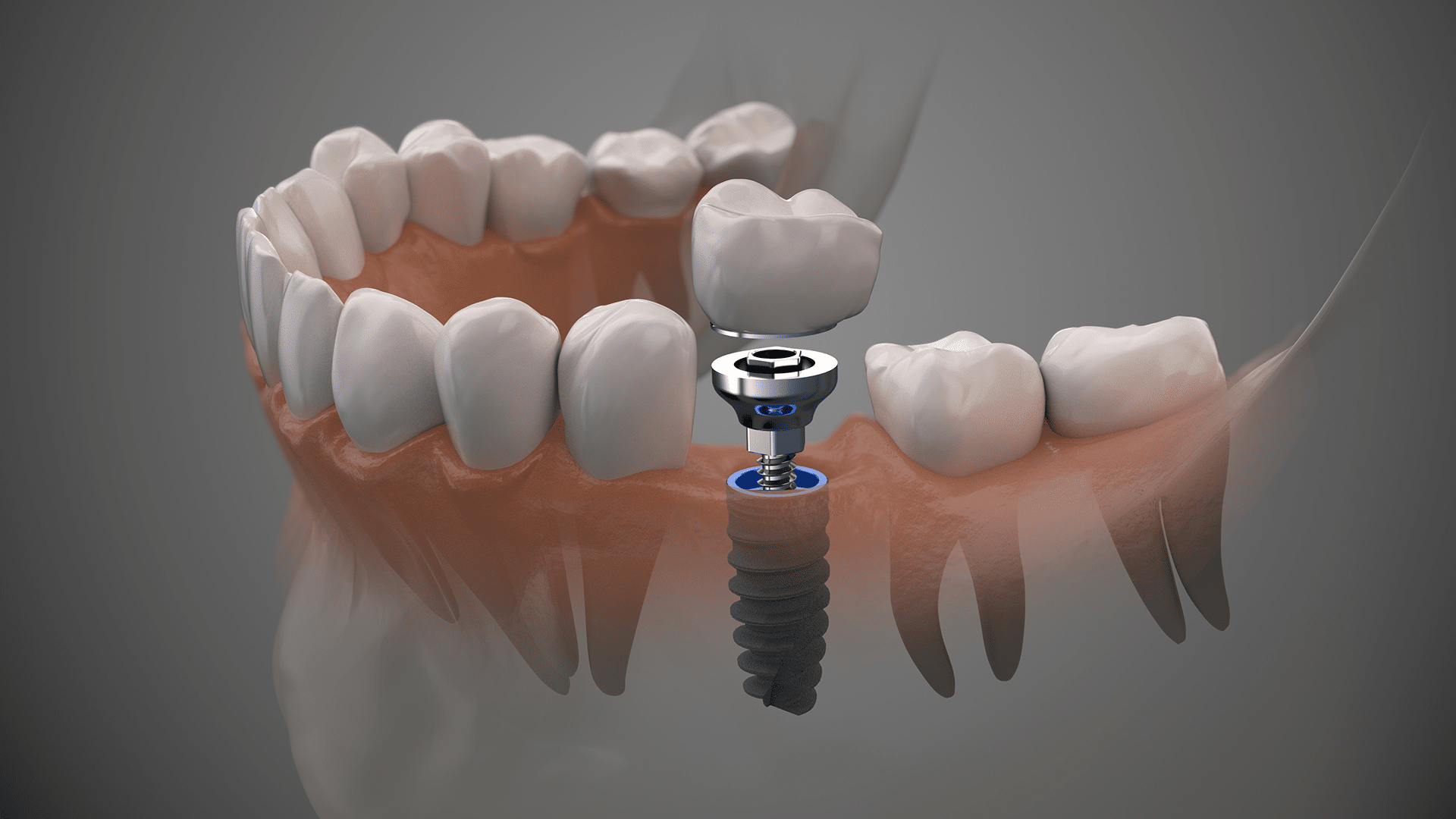
Why Dental Implants may be for you!
KM Admin
Are you missing one or more teeth? Dental implants may be the answer you’ve been searching for. They not only restore your ability to eat, speak, and smile with confidence but also provide a permanent solution that looks and feels like natural teeth. Here are seven common reasons why people choose dental implants as their...read more

Top 6 Invisalign® Questions and Answers: Everything You Need to Know
KM Admin
If you’re considering straightening your teeth, Invisalign® is a popular and effective orthodontic treatment to consider. However, our Alexandria dentist, Dr. Mullaney, understands you may have some questions before making a decision about treatment. Here are the top six questions she gets about Invisalign® treatment. What to Know About Invisalign® Invisalign® is a brand...read more











